Neuropathy Treatment: Choosing the Best Medication for You
Millions of individuals suffer with neuropathy, which causes pain, tingling, numbness, and muscular weakness. It may cripple everyday life, making even ordinary tasks difficult. Neuropathy may be caused by diabetes, chemotherapy, infections, and autoimmune diseases. Effective symptom management begins with knowing the illness since the underlying cause determines the appropriate therapy. Medication helps neuropathy patients feel better and live better.
Understanding drugs and how they function may help people choose the best therapy for their ailment. Finding the correct balance between efficacy and tolerability is vital since everyone reacts differently to drugs. Some nerve pain drugs directly target nerves, while others alter brain pain signals. Exploring the most effective drugs and their processes may help neuropathy sufferers control symptoms and enhance quality of life.
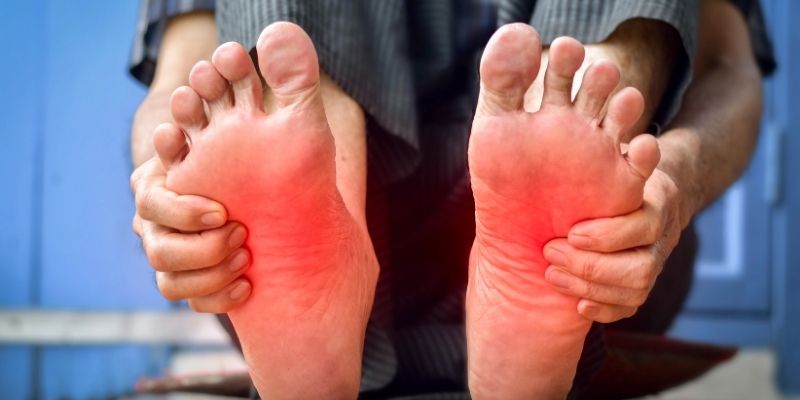
Neuropathy Causes and Understanding
Damage to nerves outer the brain and spinal cord causes peripheral neuropathy. The most typical symptoms are scorching pain, tingling, muscular weakness, and response loss, depending on the nerves involved. These symptoms generally start in the hands and feet before spreading to other regions of the body, called "glove and stocking" neuropathy. The pain might range from severe and shooting to prolonged numbness or hypersensitivity to touch. Mobility and coordination may be severely impaired by severe neuropathy, making ordinary chores challenging.
Sensory, motor, and autonomic nerves comprise the nervous system. Motor nerves govern muscular movement, whereas sensory nerves control pain and temperature. Blood pressure and digestion are controlled by autonomic nerves. Different symptoms and problems may result from neuropathy affecting one or more of these nerve types. Knowing the nerve type helps decide the best therapy. After treating the underlying illness, certain instances of neuropathy may need long-term medication and lifestyle adjustments.
Diabetes is the most dominant cause of neuropathy. Nearly 50% of diabetics get diabetic neuropathy due to high blood sugar levels damaging nerves. Vitamin deficiencies, especially B12, and prolonged drinking may induce nerve injury owing to inadequate nutrition. Nerve irritation and discomfort may result from autoimmune illnesses like lupus and rheumatoid arthritis. HIV, Lyme disease, and shingles may directly harm nerve tissue. Cancer treatments and other medications may damage neurons, and renal diseases can cause blood toxin accumulation. Identifying the reason is vital since it determines the best therapy for symptoms.
Neuropathy antidepressants are first-line.
Before discussing drugs, remember that neuropathy therapy is very customized. One person's solution may not work for another. However, nerve pain-relieving medicines are usually first-line therapy. Antidepressants change how the nervous system interprets pain signals, alleviating neuropathic pain. These drugs are generally taken at lower dosages than depression drugs and may help many people without affecting their mood.
Neuropathy is often treated with tricyclic antidepressants (TCAs) such as amitriptyline and nortriptyline. Blocking serotonin and norepinephrine reuptake increases their nervous system availability, modulating pain perception. TCAs greatly alleviate neuropathic pain by changing spinal cord and brain nerve transmission. However, adverse symptoms include tiredness, dry mouth, dizziness, constipation, and weight gain, which may restrict their usage in certain people. Serotonin-norepinephrine reuptake inhibitors (SNRIs) like duloxetine (Cymbalta) act similarly but have fewer negative effects. SNRIs may also enhance mood and well-being for chronic pain patients with depression.
Anticonvulsants: A Popular Alternative
Doctors use anticonvulsants if antidepressants fail or have negative effects. These medications were intended to treat epilepsy, but they also work effectively for neuropathic pain. Anticonvulsants stabilize nerve activity, inhibiting pain-causing nerve transmission. They help with diabetic neuropathy, post-herpetic neuralgia, and spinal cord injury-related neuropathic pain.
The most widely prescribed neuropathy anticonvulsants are gabapentin (Neurontin) and pregabalin (Lyrica). Gabapentin calms hyperactive nerves, relieving pain, but pregabalin is more powerful and requires smaller dosages. Although well-tolerated, these drugs might cause dizziness, weariness, weight gain, and brain fog. Patients may need many weeks to get full effects from these drugs, so persistence is crucial. Doctors may start patients on a low dosage and gradually raise it to reduce negative effects.
Tramadol and Opioids: Second-Line Treatments
If first-line therapies fail, opioids and tramadol may be used. Due to reliance and negative effects, these medicines are reserved for severe neuropathic pain. Opioids may relieve pain, but they should only be taken under medical supervision to avoid tolerance.
Tramadol, a centrally acting painkiller, binds to brain opioid receptors and norepinephrine reuptake and inhibits serotonin. Its dual action makes it a unique painkiller. Oxycodone and morphine, although frequently utilized, are not recommended for long-term therapy because of their dependence potential. Opioids may cause nausea, sleepiness, constipation, and respiratory depression, making them unsuitable for persistent neuropathic pain.
Topicals: A Different Approach
For people who avoid systemic drugs, topical pain alleviation is localized. Chili pepper-derived capsaicin cream is a popular painkiller that depletes substance P, a pain-signaling molecule. Though it burns, capsaicin cream may relieve localized nerve pain with regular application.
Numbing lidocaine patches are another topical therapy. These patches assist with localized pain like post-herpetic neuralgia. Topical therapies have fewer systemic adverse effects than oral drugs, making them preferable for certain patients. For best results, they may need to be used with other therapies.
Supplementing Drugs with Non-Pharmaceuticals
While drugs are essential for neuropathy management, non-pharmacological therapy may help. Physical therapy reduces pain, strengthens muscles, and improves circulation. Another prominent alternative treatment for neuropathic pain is acupuncture. These therapies may complement medicine to manage pain better.
Lifestyle and dietary adjustments may help manage neuropathy symptoms. Patients with diabetic neuropathy must maintain steady blood sugar levels. Vitamins B12 and alpha-lipoic acid help improve nerve health. These methods may improve pain alleviation and well-being when used with medicine.

Choosing Your Best Treatment
Choosing the appropriate neuropathy medicine might be difficult with so many possibilities. Working with a doctor to find the best treatment for your symptoms, medical history, and lifestyle is crucial. Patient and persistent trial and error may lead to successful medicine.
In conclusion, neuropathy is difficult and needs individualized therapy. Understand your drug choices and work with a doctor to identify the best one for controlling symptoms and enhancing quality of life. Neuropathy treatment requires perseverance and patience, since there is no one remedy.
Conclusion
Neuropathy demands individualized therapy due to its complexity and debilitating nature. Neuropathy may be caused by diabetes, autoimmune illnesses, pharmaceutical side effects, and infections, so selecting the proper treatment is crucial to controlling symptoms. Antidepressants and anticonvulsants are usually the best first-line therapy; however, some individuals may need opioids or topical medicines.
Finding the best neuropathy therapy is difficult since everyone reacts differently to drugs. Patiently following therapy, monitoring symptoms, and working with a doctor may improve pain management and quality of life. Lifestyle adjustments, physical therapy, and other therapies may improve symptoms. Neuropathy may be incurable, but the appropriate therapy may restore function, alleviate discomfort, and enhance well-being.